Breast Reconstruction
Home/Breast Reconstruction
Home/Breast Reconstruction
The breast is the most common site of cancer in American women and breast cancer will develop in 1 of every 8 to 9 women in their lifetime. Although a cure has not yet been found, breast cancer is now detected earlier and there are now improved modes of treatment. Still, being diagnosed with breast cancer is frightening, confusing and earth shattering. Our team at Parva Plastic Surgery sees the hope, determination and personal victories in the lives of our many breast cancer patients.
Women are often faced with decisions and feel ill-prepared to make them. Some important questions they have to ask themselves include:
“Dear Dr. Parva,
I wanted to thank you so very much for all of your wonderful care! I just celebrated my 10 year anniversary last Friday. All of your talents and ‘thoughtfulnesses’ are so very much appreciated.”
Statistically, only 35% of women with breast cancer undergo breast reconstruction. Unfortunately, that is not by choice, but most often because many women are not aware of reconstruction and the options available to them. States have begun passing legislation that requires all women with a diagnosis of breast cancer to be referred to a Plastic Surgeon so they can be informed of their individual options. Regardless of legislative efforts, as Plastic Surgeons committed to the care of our breast cancer patients, we have an obligation to increase public awareness and to expand physician awareness so breast cancer patients receive optimal, individualized care.
Women who have undergone breast reconstruction have said that the procedure alleviates the pain of losing a breast and improves their self-esteem and self-confidence. In fact, many can begin the breast reconstruction process at the time of a mastectomy, therefore minimizing the feeling of loss associated with a mastectomy. Conversely, other women may choose to proceed with breast reconstruction months or even years after their mastectomy (delayed reconstruction). With the many options and advances available today, every woman diagnosed with breast cancer should seriously consider her reconstructive options, as well as the cancer treatment options.
Some common myths about breast reconstruction should be clarified:
The importance of consulting witih a plastic surgeon during the time of breast cancer diagnosis.
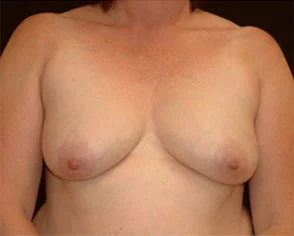
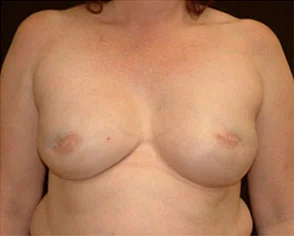
This active, healthy 50 year-old mother of three was found to have a right breast mass. On further evaluation, she in fact had breast cancer involving both breasts. She had bilateral skin and areola-sparing mastectomies and 2-stage breast reconstruction. She had 550cc Moderate Plus Profile silicone gel implants and is seen 9 months after the second stage reconstruction. She decided not to have a nipple reconstruction.
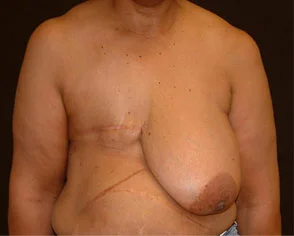
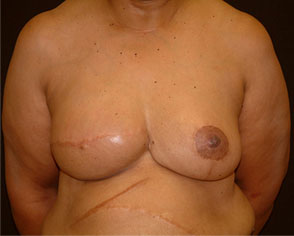
This young woman was diagnosed with right breast cancer at the age of 57. She had a mastectomy at that time, deciding not to have breast reconstruction. One year later she began her delayed breast reconstruction by having a tissue expander placed. The left breast was reduced for symmetry and to relieve her of the significant imbalance in upper body weight distribution. Five months later, the right breast tissue expander was replaced with a 750cc saline implant.
For optimal care and results our Virginia plastic surgeon, Dr. Parva, strongly supports referral to a Board Certified Plastic Surgeon for everyone diagnosed with breast cancer. Even if the desire is for breast conservation, such as lumpectomy and radiation, coordinated care between the team of breast surgeon and plastic surgeon can optimize the final outcome in treating the cancer and achieving the best aesthetic appearance of the breast.
To guide you in your decision making, Dr. Parva will help you process common questions such as:
If a patient decides they are interested in breast reconstruction, Dr. Parva will provide a detailed explanation of their options, including the pros and cons of each technique. There are two main types of breast reconstruction, both of which can provide beautiful results for the right candidates.
Tissue flap breast reconstruction uses the patient’s own tissue to recreate the projection and appearance of the natural breast mound. This harvested tissue is often taken from areas like the abdomen, buttocks, or back. The various tissue flap techniques can be performed alone or in combination with implant reconstruction.

Breast implant reconstruction uses saline or silicone gel breast implants to rebuild the breast following mastectomy. Various implant types are available and can effectively restore the natural breast appearance.

After the breast mound has been reconstructed, whether through the flap or implant technique, nipple reconstruction can provide the finishing touch by recreating the appearance of the nipple and areola. This procedure is often paired with nipple and areola tattooing, though most of our patients opt to only receive tattooing.
The recovery after breast reconstruction will vary based on whether a flap technique and/or breast implants are utilized, as well as if any secondary breast reconstruction procedures are performed. In general, patients can expect some swelling and soreness at the beginning of their recovery, which should gradually dissipate over several days. Discomfort is typically mild and can be managed with oral pain medication. Immediately after surgery, patients are placed in a support bra or bandage to facilitate healing.
Most women feel comfortable enough to return to their normal daily activities within about one to two weeks. However, strenuous activities should be avoided for at least six weeks to allow the breast and possible donor site to heal. Patients will be given post-operative care instructions prior to their surgery to help them navigate their recovery. In addition, follow-up visits will be scheduled with Dr. Parva, allowing him to monitor the patient’s healing progress.
If any questions or concerns arise during the recovery process, Dr. Parva encourages patients to contact our office.
Please contact Parva Plastic Surgery for your breast reconstruction consultation with Dr. Parva, board certified plastic surgeon, today.